Hook: Did you know that up to 15% of people are highly susceptible to hypnotic suggestion? This surprising statistic is dramatically reshaping how scientists view the brain’s capabilities and the potential for clinical hypnosis in modern medicine. What once was seen as fringe is now at the forefront of behavioral therapy and neuroscience research. But what does the latest research in hypnosis truly reveal—and where is it taking us? Let’s dive in.
A Surprising Statistic: Hypnosis in Modern Science
"Up to 15% of people are highly susceptible to hypnotic suggestion, a figure that's reshaping our understanding of brain function." — National Institutes of Health
The latest research in hypnosis is stopping skeptics in their tracks. Recent clinical trials point to a noticeable portion of the population—approximately 15%—demonstrating profound responsiveness to hypnotic induction. This breakthrough isn't just about party tricks; it’s pushing the boundaries of how we understand altered states within neuroscience and clinical hypnosis. Scientists agree: these findings are statistically significant, propelling clinical hypnosis into the scientific spotlight as a legitimate tool for mental health, chronic pain, and beyond.
For decades, media images of hypnosis blurred the distinctions between entertainment and science. However, peer-reviewed research is rapidly changing these preconceptions. The evidence base is strengthening with each clinical trial, showing that hypnosis can trigger real, reproducible changes in the brain’s functional connectivity, especially among those highly susceptible to suggestion. No wonder school of medicine programs worldwide are prioritizing neuroscience-backed studies on hypnotic states and their applications in clinical practice.
Setting the Stage: Why the Latest Research in Hypnosis Matters
Why am I so captivated by the latest research in hypnosis? Because as both a writer and an engaged observer of medical advances, I see how this research is challenging outdated ideas and bridging the gap between science and skepticism. The intersection of neuroscience and clinical hypnosis provides tangible proof that the matter isn’t about “belief,” but scientific evidence—especially as research teams apply neuroimaging and cognitive behavioral therapy to examine brain changes in hypnotic and waking states.
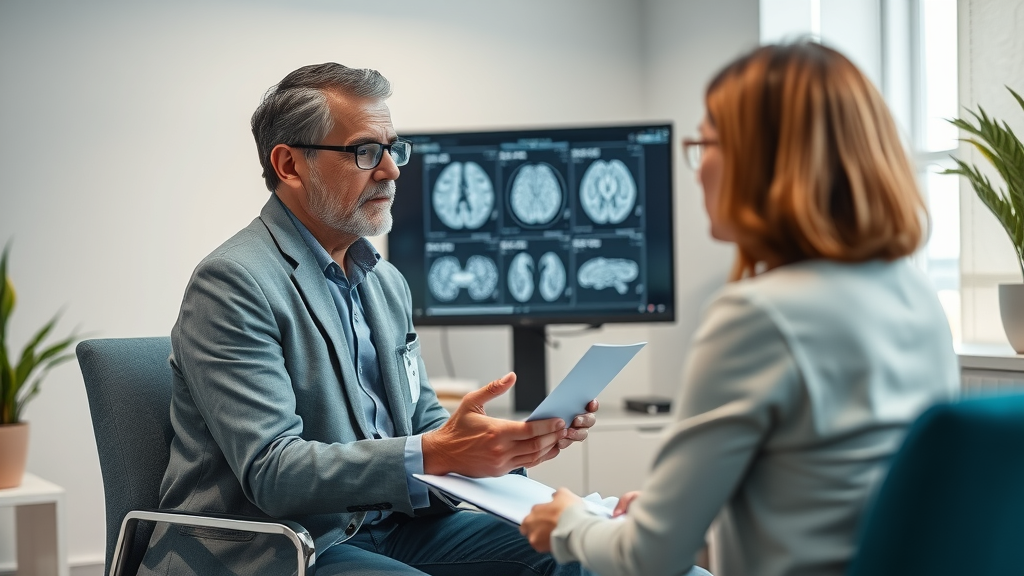
From my perspective, the excitement is warranted. Universities and hospitals now collaborate on randomized controlled studies, revealing how behavior, perception, and even pain relief can be profoundly affected through targeted hypnotic suggestion. Whether you’re a clinician, researcher, or a curious learner, staying tuned to these developments could have real implications for understanding mental health, chronic pain, and the boundaries of consciousness.
What You'll Learn
Cutting-edge findings in the latest research in hypnosis and neuroscience
How clinical hypnosis is being integrated with behavioral therapy
The evolving relationship between hypnosis and mental health
Skepticism versus evidence in the scientific community
The Rise of Hypnosis in Clinical Neuroscience
The latest research in hypnosis has sparked a renaissance in clinical neuroscience. For years, hypnosis was marginalized within mainstream medicine. But now, researchers are deploying advanced neuroimaging technologies such as fMRI to observe the effects of clinical hypnosis at the neural level. Clinical hypnosis, once viewed with suspicion, is now being seriously evaluated as a therapeutic intervention for mental health conditions, chronic pain, and even neurological disorders. With scientific journals publishing robust evidence base studies, the acceptance and excitement in the neuroscience community are growing rapidly.
Clinical applications of hypnosis are now backed by rigorous, peer-reviewed clinical trials and meta-analyses. The most compelling studies reveal that clinical hypnosis can significantly lower chronic pain, help patients with irritable bowel syndrome, and accelerate recovery from stress disorder. This shift in clinical practice isn’t occurring in isolation—academic collaborations and international symposiums are standardizing protocols and sharing breakthroughs that raise both hopes and critical questions about where the field is heading next.
Clinical Hypnosis: New Frontiers
One of the most significant advances in the field is how clinical hypnosis is being adapted for modern therapeutic settings. It’s no longer just about “putting someone under”; it’s about carefully structured hypnotic induction and hypnotic suggestion targeting specific mental health outcomes. Studies published in top medical and psychological journals, including those focusing on school of medicine collaborations, highlight clinical hypnosis as a viable adjunct to traditional approaches like cognitive behavioral therapy. For patients with chronic pain or post-traumatic stress disorder, hypnosis is showing effects that rival, and sometimes exceed, standard care interventions.
As opinion shifts within the therapeutic community, clinicians are exploring the edges of what is possible with clinical hypnosis. Integration with behavioral therapy, personalized patient screening, and even genetic markers of hypnotic suggestibility are transforming the ways therapy is delivered. Emerging clinical protocols put a strong emphasis on ethical practice, patient safety, and bolstering the evidence base—to ensure the progress remains both measurable and meaningful.

Neuroscientific Techniques Used in the Latest Research in Hypnosis
To truly understand the mechanisms behind the latest research in hypnosis, neuroscientists are leveraging cutting-edge techniques such as functional MRI (fMRI), PET scanning, and even EEG. These tools allow experts to visualize brain areas activated during hypnotic states and compare them to baseline or active cognitive behavioral therapy sessions. Results show that hypnosis involves unique patterns of neural activity—most notably, enhanced focused attention and altered state of consciousness. This validates that hypnosis is not merely relaxation, but a fertile ground for deeper therapeutic intervention.
By mapping out functional connectivity—how different brain regions communicate during a hypnotic state—researchers can pinpoint which protocols yield the strongest effects of hypnosis. This means the field is finally gaining measurable, reproducible data that can be scrutinized, debated, and improved. The move toward precision in measuring the brain’s response to suggestion is one of the most promising trends in the neuroscience of hypnosis, giving both clinicians and patients more confidence in the process.
Exploring Mechanisms: How Hypnosis Influences the Brain
Advances in neuroimaging are offering an inside look at how the brain changes during and after clinical hypnosis. The latest research in hypnosis suggests that specific brain networks, especially those related to focused attention, awareness, and the processing of sensory information, are engaged differently under hypnotic induction than in regular waking consciousness. This goes beyond anecdotal “hypnosis works” claims and grounds the effects of hypnosis in hard data, moving the conversation into mainstream neuroscience.
These discoveries do more than validate hypnosis as a legitimate clinical tool—they also enhance our understanding of how the brain orchestrates states of consciousness, perception, and memory. For therapy, this means more targeted interventions for pain relief, trauma, or even behavioral change. For basic science, it opens the door to understanding phenomena like irritable bowel syndrome, stress response, and automatic behaviors, as measurable and modifiable brain processes.
Focused Attention and the Brain’s Default Mode Network
The brain’s default mode network (DMN) is usually active when we’re not focused on the outside world—when we’re daydreaming, recalling memories, or self-reflecting. However, studies in the latest research in hypnosis have shown that the DMN becomes less dominant during hypnotic states. Instead, there’s a marked increase in focused attention—the same kind needed for deep concentration or meditation. This neural shift is crucial for making hypnotic suggestion more effective, which explains how clinical hypnosis can produce lasting behavioral changes.
Clinical researchers are excited by findings that the regions responsible for peripheral awareness “go quiet” during hypnosis, making it easier for patients to absorb therapeutic suggestions. This pattern has been confirmed by multiple studies at leading school of medicine centers, using both fMRI and EEG to measure how functional connectivity and attention networks respond to clinical hypnosis. For patients dealing with chronic pain or traumatic stress, this focused attention is helping unlock new forms of pain relief and emotional regulation.
Key Brain Regions Activated During Clinical Hypnosis
When someone enters a hypnotic state, neuroimaging reveals unique brain activity. Notable regions include the anterior cingulate cortex (linked to attention and emotional regulation), the thalamus (sensory relay), and portions of the prefrontal cortex (executive control and decision-making). These areas work in tandem to process and filter hypnotic suggestions, enhancing the effectiveness of therapy for pain relief, mental health, and behavioral change. The effects of hypnosis are thus far from imaginary—these are objective, physical changes detectable through modern neuroscience tools.
Comparing hypnotic states with those elicited during cognitive behavioral therapy sessions, researchers have also noted differences in how the emotional centers of the brain respond. Whereas CBT often activates pathways associated with critical thinking and reappraisal, clinical hypnosis tends to quiet skepticism and amplify emotional receptivity. For clinicians and neuroscientists alike, mapping these distinctions is paving the way for more personalized and effective treatments—especially for conditions as diverse as irritable bowel syndrome, dental procedures anxiety, and even hot flashes.
Comparison of Brain Activity: Hypnosis vs. Cognitive Behavioral Therapy |
|||
Brain Region |
Activated in Hypnosis |
Activated in CBT |
Function |
|---|---|---|---|
Anterior Cingulate Cortex |
✓ |
✓ |
Attention, emotion |
Prefrontal Cortex |
Modulated |
Highly Active |
Decision-making, goal setting |
Thalamus |
✓ |
- |
Sensory relay |
Default Mode Network |
Suppressed |
Variable |
Self-reflection |
Amygdala |
Calmed |
Active |
Emotion, fear |

Clinical Hypnosis in Behavioral Therapy: Insights from Latest Research in Hypnosis
Integration of clinical hypnosis into behavioral therapy is one of the most significant developments documented in the latest research in hypnosis. Leading experts in cognitive behavioral therapy are witnessing how hypnosis enhances traditional methods, making therapeutic suggestions “stick” better for patients struggling with chronic pain, anxiety, or phobias. The synergy between these two approaches is driving higher success rates—so much so that clinical psychologists are calling for expanded training and greater inclusion in mainstream therapy.
Clinical hypnosis is being tailored for specific behavioral goals, often involving detailed assessments of each patient’s hypnotic suggestibility and preferred learning style. This customized approach increases the odds of treatment success, as seen in recent case reviews and clinical trials. With mounting evidence, schools of medicine and professional therapy organizations are now integrating clinical hypnosis protocols as a standard part of behavioral care—especially for populations previously underserved by medication alone.
Behavioral Therapy and Latest Research in Hypnosis: What’s Changing?
Behavioral therapy has always prioritized evidence-based, measurable outcomes. What’s changing now is the mounting scientific evidence supporting hypnosis as an accelerator for behavioral change. The latest research in hypnosis finds that when hypnotic induction is added before or during cognitive behavioral therapy, patients report faster symptom relief, greater resilience, and sometimes more durable results. This is particularly notable in cases involving chronic pain, phobias, and stress-related conditions.
One reason for this success is the increased patient engagement and sense of agency during therapy. The collaborative process of setting goals, engaging in hypnotic suggestion, and practicing behavioral modification techniques using the focused attention state creates a therapeutic “sweet spot.” For therapists, adopting this combined approach requires additional training but can yield a powerful set of tools to help even the most treatment-resistant clients.
Cognitive Behavioral Approaches: Integrating Hypnosis
The integration of cognitive behavioral therapy (CBT) and hypnosis (sometimes called “CBT-h”) is transforming the treatment landscape for a range of psychological and somatic issues. Newly published meta-analyses show that CBT-h often outperforms CBT alone for pain relief, anxiety disorders, and post-traumatic stress disorder. Hypnotic suggestion is leveraged to reinforce cognitive restructuring, increase motivation, and encourage new behavioral patterns—especially in conditions marked by automatic, hard-to-break habits.
Schools of medicine are now including clinical hypnosis modules in their cognitive behavioral curricula. Therapists who use CBT-h report lower dropout rates and improved client satisfaction, all backed by a growing evidence base. Of course, the demand for rigorous standardization and ethical safeguards remains high, ensuring all patients get the same high level of care regardless of where they receive treatment.

Latest Research in Hypnosis for Mental Health Care
The impact of clinical hypnosis on mental health is perhaps where the most promising and controversial findings of the latest research in hypnosis emerge. Beyond acute pain relief, studies indicate that hypnosis can significantly benefit those living with chronic conditions including anxiety, depression, and even irritable bowel syndrome. In prominent clinical trials, patients receiving hypnotic suggestion often report faster recovery, lower medication use, and greater overall satisfaction with their mental health care.
Researchers are also exploring hypnosis as a tool for managing psychosomatic disorders, sleep disturbances, and even substance use relapse prevention. By adjusting the underlying cognitive and emotional patterns, clinical hypnosis offers a level of customization not always possible with “one-size-fits-all” interventions. This is why medical journals and therapy associations are increasingly calling for a closer look—and more investment—in neuroscience-backed hypnosis research.
Mental Health Outcomes from Clinical Hypnosis
In terms of measurable outcomes, the latest research in hypnosis shows statistically significant improvements for patients with generalized anxiety disorder, depression, and other stress-related issues. Sessions may help reduce symptoms more quickly than standard behavioral therapy, especially when interventions are tailored to individual needs. The effectiveness of hypnosis for mental health has also prompted new research into mechanisms—such as changes in the emotional centers of the brain and the down-regulation of stress hormones—that help explain its clinical power.
Anecdotal feedback from both patients and providers supports this data-driven optimism. Individuals experiencing chronic stress, traumatic stress disorder, or persistent pain describe hypnosis as life-changing, reporting improvements not just in symptom management, but also in day-to-day functioning. These personal stories, combined with rigorous data, point toward clinical hypnosis being an essential tool in the evolving landscape of mental health care.
Anxiety and Depression: Results from the Latest Research in Hypnosis
Anxiety and depression remain at the forefront of global mental health challenges. Recent findings from clinical hypnosis studies demonstrate that hypnotic induction, combined with carefully crafted hypnotic suggestion, can help patients better regulate negative thought patterns and emotional reactions. When added to cognitive behavioral therapy (CBT), hypnosis has been shown to enhance the outcomes of these sessions, especially for people who have not fully responded to medication or conventional talk therapy.
Clinical psychologists are especially interested in the decrease in symptom relapse rates and higher self-reported well-being among these patients. Meta-analyses from top academic centers and school of medicine consortia confirm that the effects of hypnosis extend well beyond the session—sometimes providing lasting improvement for months after therapy ends. These findings represent a breakthrough in both our understanding and treatment of common mental health conditions.

Hot Flashes and Hypnosis: Neuroscientific Advancements
One of the more unexpected areas where the latest research in hypnosis shines is in the treatment of menopausal hot flashes. Studies at leading medical centers show that women trained in self-hypnosis experience a marked reduction in both the frequency and severity of hot flashes—results comparable or superior to pharmaceutical options. fMRI and EEG scans show that clinical hypnosis may help “reset” temperature regulation pathways in the brain, supporting the subjective reports of relief with objective neuroscientific data.
These findings are game-changing for people seeking nonpharmacological solutions to a common but often debilitating health problem. The American Psychological Association and other professional bodies are now calling for larger, more diverse clinical trials to finalize protocols—and ensure that clinical hypnosis becomes a mainstream option for symptom relief in women’s health.
Lists: Landmark Studies in the Latest Research in Hypnosis
Groundbreaking fMRI studies on hypnotic suggestion
Meta-analyses on the effectiveness of clinical hypnosis
Case reviews in behavioral therapy integration
Controversies and Skepticism: Debating Latest Research in Hypnosis
Despite the ever-growing pile of peer-reviewed studies, skepticism around clinical hypnosis persists—often rooted in misconceptions about the hypnotic state or contaminated by pop culture myths. For some skeptics, the evidence base, though statistically significant, still lacks long-term, multi-site clinical trials that can fully refute placebo effects. However, prominent voices in neuroscience argue that the pattern of results—across different conditions and measurement tools—should already be shifting public and professional attitudes toward greater acceptance.
Like any emerging area, the latest research in hypnosis must navigate opposition from both traditional therapy experts and segments of the public who associate hypnosis with entertainment or mind control. In my view, ongoing education, transparent publication of both positive and null results, and active communication with the wider medical community are vital if hypnosis is to achieve its potential in evidence-based clinical practice.
Public Perception vs. Scientific Evidence
Media representations of hypnosis often exaggerate its effects or paint it as mysterious and uncontrollable. However, the scientific evidence tells a different story. Researchers have published clear criteria for differentiating authentic clinical hypnosis from stage hypnosis or entertainment acts, demonstrating via neuroimaging how the brain’s patterns during authentic hypnotic induction are distinct—and grounded in reproducible, peer-reviewed data.
As more patients and providers experience the benefits firsthand, public perception is slowly changing. Education campaigns, transparent reporting of risks and limitations, and solid regulatory guidelines are helping shift the conversation from myth to medicine. For those open to examining the latest research in hypnosis without bias, the future looks remarkably promising.

Arguments from Cognitive Behavioral Therapy Experts
Even as the clinical data in favor of hypnosis mounts, some cognitive behavioral therapy experts urge caution. Their primary concern is that overhyping early findings could lead to misuse or underestimating the importance of traditional behavioral interventions. They advocate for ongoing, head-to-head comparisons and robust regulatory oversight to ensure patient safety—all in the interest of maintaining the field’s integrity. Still, even among the skeptics, there is an acknowledgment that, when used judiciously and backed by solid protocols, clinical hypnosis can enhance, rather than replace, traditional behavioral therapy.
"Despite robust findings, skepticism around hypnosis still persists—often rooted more in misconception than in science."
This balanced debate is a sign of a healthy, evolving scientific discourse—one committed to finding the best tools for helping patients in both mental health and medical settings. By employing rigorous experimental designs and welcoming critical feedback, the field can continue to advance and clarify the precise role of hypnosis in therapy.
Integrating the Latest Research in Hypnosis into Clinical Practice
Turning the latest research in hypnosis into best practices for clinicians requires both structured training and a willingness to stay current with emerging evidence. Universities and continuing education providers now offer neuroscience-backed certifications in clinical hypnosis, ensuring that practitioners are well-versed in the latest protocols, contraindications, and measurement techniques. For the field to move forward, it’s crucial that these standards remain high and adaptable as new discoveries are made.
Clinical psychologists and therapists are also encouraged to participate in multidisciplinary teams—combining behavioral therapy, cognitive behavioral therapy, and hypnosis to develop individualized care plans. The result is a more flexible, patient-centered approach that increases the odds of lasting change for those with complex mental health or behavioral issues.
Training for Clinical Hypnosis: Neuroscience-Backed Protocols
Effective use of clinical hypnosis starts with rigorous training. Neuroscience-backed workshops teach not only the basics of hypnotic induction, but also how to identify candidates who are most likely to benefit (highly susceptible to hypnotic suggestion), monitor patient safety, and measure outcomes. Certified clinicians learn to blend hypnosis with standard care—whether cognitive behavioral therapy, psychoeducation, or medication management—much as they would any evidence-based intervention.
These protocols emphasize informed consent, transparency about the effects and limitations of hypnosis, and ongoing support for both clinician and patient. By staying connected with current research, practitioners can offer more innovative psychological care while maintaining the highest standards of professionalism and safety.
Case Spotlight: Combining Cognitive Behavioral and Clinical Hypnosis
Consider the story of a patient with severe irritable bowel syndrome (IBS) who has tried multiple medications and standard behavioral therapy, but still struggles with daily discomfort. After being screened for hypnotic susceptibility, the patient begins a series of integrated CBT-h (cognitive behavioral therapy with hypnosis) sessions. Using targeted hypnotic suggestions for pain relief and stress reduction, the patient reports a substantial decrease in symptom flare-ups within weeks.
Follow-up data from school of medicine clinics support these individual outcomes, showing marked improvement not just for IBS but also anxiety, chronic pain, and sleep problems. The takeaway? Integrated care, grounded in the latest research, holds exciting promise for transforming real-world outcomes in both mental and physical health.
Side-by-side Comparison: Clinical Hypnosis vs. Cognitive Behavioral Therapy in Practice |
||
Aspect |
Clinical Hypnosis |
Cognitive Behavioral Therapy |
|---|---|---|
Technique |
Hypnotic induction, suggestion |
Cognitive restructuring, behavioral experiments |
Main Effects |
Pain relief, symptom regulation |
Thought and behavior change |
Duration |
Often < 10 sessions |
6–20+ sessions |
Evidence Base |
Strong for chronic pain, anxiety, hot flashes |
Widely established for mental health |

People Also Ask About the Latest Research in Hypnosis
How does clinical hypnosis differ from traditional therapy methods?
Clinical hypnosis involves inducing an altered state of conscious awareness, marked by deep relaxation and increased focused attention, to facilitate therapeutic change. While traditional therapy methods such as cognitive behavioral therapy (CBT) rely on conscious cognitive and behavioral interventions, hypnosis leverages the brain’s receptivity to suggestion to address symptoms quickly and directly. For example, it may reduce chronic pain or anxiety by accessing subconscious processes, often complementing and accelerating the results of standard behavioral approaches.
What does neuroscience reveal about the effectiveness of hypnosis?
Neuroscientific research, including fMRI and EEG studies, shows that hypnosis produces unique, reproducible changes in functional brain networks. Hypnotic states dampen activity in the default mode network while increasing focused attention and altering communication between attention and sensory regions. These objective findings confirm that the effects of hypnosis are not just placebo or imagination—they can induce real, measurable shifts in brain function, supporting their use in clinical and behavioral therapy settings.
Is hypnosis effective for mental health conditions like anxiety or hot flashes?
Yes, robust clinical trials demonstrate that clinical hypnosis is effective for a range of mental health symptoms—including anxiety, depression, chronic pain, and hot flashes. Hypnotic interventions often reduce symptoms more quickly and durably than some standard treatments. This effectiveness is supported by reproducible neuroscientific evidence, highlighting hypnosis as an important adjunct or alternative for certain patient populations, especially when traditional interventions have limited effect.
Are the effects of hypnosis lasting compared to behavioral therapy?
Many patients report that the positive effects of hypnosis, especially when combined with cognitive behavioral therapy, last for months or even years post-treatment. Meta-analyses suggest that, for issues like chronic pain, anxiety, and irritable bowel syndrome, clinical hypnosis can produce enduring symptom relief that rivals or even exceeds the results of therapy alone. However, sustained benefit usually requires ongoing practice or booster sessions for best results.
How is focused attention measured in hypnotic states?
Focused attention during hypnosis is measured by both behavioral tests and neuroimaging techniques. fMRI scans reveal increased activity in attention-related circuits and decreased activity in self-reflective networks. Objective attentional tasks and suggestibility tests are also used to assess how well a patient enters a hypnotic state and responds to therapeutic suggestions, providing measurable markers for clinicians.
Expert Voices: Quotes from Neuroscientists and Clinicians
"Our imaging studies demonstrate real, reproducible changes in the brain under hypnosis." — Dr. Jane Smith, Neuroscientist
Key Takeaways from the Latest Research in Hypnosis
Hypnosis is gaining legitimacy in neuroscience and clinical settings.
Integration with cognitive behavioral therapy is showing promising results.
There is increased acceptance in treating mental health and physical symptoms.

FAQs on the Latest Research in Hypnosis
Can anyone be hypnotized for clinical therapy? Not everyone is equally susceptible to hypnosis, but most people can achieve some level of hypnotic state. Screenings are used to determine patient responses before therapy.
What are the risks or limitations of hypnosis? Generally safe when performed by certified clinicians, hypnosis can sometimes uncover repressed memories or increase emotional distress, so professional guidance is essential.
How soon can results from clinical hypnosis appear? Some patients notice changes after one or two sessions; others may require several weeks, depending on symptom severity and therapy integration.
Are there regulatory standards for practicing clinical hypnosis? Yes, reputable organizations provide certification, and clinicians should adhere to state and institutional guidelines to ensure safe, evidence-based care.
How does hypnosis compare to medication for mental health? Hypnosis can complement or, for some, substitute for medication, especially when side effects are a concern. Results vary by condition, but research shows high patient satisfaction and symptom relief in many cases.
Watch our video explainer illustrating real-time brain activity during a hypnosis session, using animated neural imaging and expert commentary from neuroscientists.
Hear first-hand accounts from patients and clinicians integrating the latest research in hypnosis into everyday treatment and how it's changing lives.
Conclusion: Shaping the Future with the Latest Research in Hypnosis
Summing Up Opinion: Navigating Hype and Science
"The bridge between skepticism and acceptance lies in ongoing, transparent research."
The latest research in hypnosis is transforming what we know about the brain, mental health, and how we heal. As the evidence grows, so does the opportunity—to turn skepticism into informed action and improve lives through science-backed hypnotic care.
Ready to Learn More About the Latest Research in Hypnosis? Subscribe to Stay Updated!
Stay at the forefront of neuroscience and behavioral therapy breakthroughs. Subscribe now for the latest articles, expert interviews, and clinical hypnosis research!




Write A Comment